Uterine fibroids (myomas, leiomyomas, or fibromyomas) are the most frequent tumors of the female genital tract: 20 to 40% of women of childbearing age have a fibroid. Fibroids range in size from very tiny to the size of an orange or larger. In some cases, they can cause the uterus to grow to the size of a five-month pregnancy or more.
Women aged between 30 and 50 are the most likely to develop fibroids. Overweight and obese women are at significantly higher risk of developing fibroids, compared to women of normal weight.
- Heavy, prolonged menstrual periods and unusual bleeding, sometime with clots. This might lead to anemia.
- Lower abdomen, back or leg pain
- Lower abdominal pressure or heaviness
- Bladder pressure leading to a constant urge to urinate
- Pressure on bowel, leading to constipation and bloating
- Abnormally enlarged abdomen
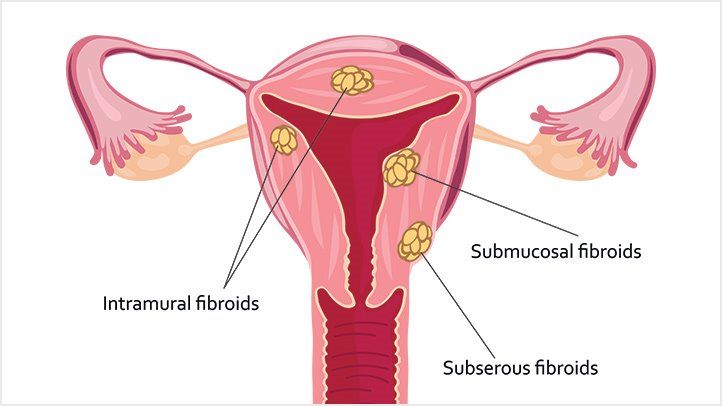
They are named according to their location within the uterus:
Intramural fibroids are located within the wall of the uterus and are the most common type; unless large, they may be asymptomatic. They may cause heavy bleeding with clots. With time, intramural fibroids may expand inwards, causing distortion and enlargement of the uterine cavity.
Subserosal fibroids are located on surface of the uterus and can become very large. They can cause pressure over bladder and rectum producing symptoms like urgent urination and constipation with back pain.
Submucosal fibroids are located in the muscle beneath the endometrium of the uterus and distort the uterine cavity; even small lesion in this location may lead to bleeding and infertility.
Cervical fibroids are located in the wall of the cervix (neck of the uterus). They may also cause infertility if obstructing the cervical canal and difficulty in normal delivery.
Fibroids are usually suspected during a gynecologic examination. The presence of fibroids is most often confirmed by a lower abdomen ultrasound scan. Fibroids can also be confirmed using MRI (magnetic resonance imaging). It is a good idea to have an MRI Scan before any kind of treatment. These imaging techniques serve as a baseline examination for follow-up after uterine fibroid embolization (UFE) or any other treatment.
Picture A. Ultrasound image shows sub mucosal fibroid Picture B. MRI image shows multiple intramural fibroids.
ComplicationsAlthough uterine fibroids usually aren’t dangerous, they can cause discomfort and may lead to complications such as anemia from heavy blood loss.
Urinary tract infections: – if pressure from the fibroid prevents the bladder from fully emptying
Pregnancy and fibroids: – Fibroids usually don’t interfere with conception and pregnancy. However, it’s possible that fibroids could distort or block your fallopian tubes, or interfere with the passage of sperm from your cervix to your fallopian tubes. In other cases, treatment for fibroids during pregnancy isn’t necessary. A common complication of fibroids during pregnancy is localized pain, typically between the first and second trimesters. This is usually easily treated with pain relievers. But sometimes in presence of fibroids one may experience repeated pregnancy losses and no other cause of miscarriage can be found.
Doctors don’t know the cause of uterine fibroids, but research and clinical experience point to these factors:
Genetic alterations: – Many fibroids contain alterations in genes that are different from those in normal uterine muscle cells.
Hormones: – Estrogen and progesterone, two hormones that stimulate development of the uterine lining during each menstrual cycle in preparation for pregnancy, appear to promote the growth of fibroids. Fibroids contain more estrogen and progesterone receptors than do normal uterine muscle cells.
Other chemicals: – Substances that help the body maintain tissues, such as insulin-like growth factor, may affect fibroid growth.
There’s no single best approach to uterine fibroid treatment. Many treatment options exist.
Watchful waiting: Many women with uterine fibroids experience no signs or symptoms. If that’s the case for you, watchful waiting (expectant management) could be the best option. Fibroids aren’t cancerous.
Medications: They help in reducing mild symptoms but do not treat the fibroids.
Non-surgical: – A. Uterine artery embolization B. HIFU
Surgical: – A. Hysterectomy B. Myomectomy
MedicationsMedications for uterine fibroids target hormones that regulate your menstrual cycle, treating symptoms such as heavy menstrual bleeding and pelvic pressure. They don’t eliminate fibroids. Medications include:
(GnRH) Agonists-Releasing Hormone. Medications called GnRH agonists treat fibroids by causing your natural estrogen and progesterone levels to decrease, putting you into a temporary postmenopausal state. Many women have significant hot flashes while using this medication.
Androgens. This drug similar to male hormone testosterone may effectively stop menstruation, correct anemia. However, this drug is rarely used to treat fibroids. Unpleasant side effects, such as weight gain, feeling depressed, anxious or uneasy, acne, headaches, unwanted hair growth, and a deeper voice, make many women reluctant to take this drug.